IDEALS
International Disaster & Emergency Aid with Long-term Support
At IDEALS, our dedicated teams work swiftly to provide life-saving care during emergencies, and our commitment extends long after the crisis has passed, rebuilding communities and restoring dignity.
About Us
Committed to Compassion & Care IDEALS was established to help relieve poverty, distress and suffering in any part of the world affected by conflict and/or natural disaster. Since 2000 we have worked extensively in Bosnia-Herzegovina, Sri Lanka, Pakistan and, more recently, in Lebanon and the occupied Palestinian territory, with the aim of providing humanitarian aid on a sustainable basis, forging links between emergency relief and long-term development. With the technical expertise available to us we have channelled our resources into the health sector: the provision of primary and secondary health care services in emergencies; the rehabilitation of health infrastructure (both buildings and equipment); the training of health workers (both hospital and community based); public health interventions; and the improvement of rehabilitation services for those with disabilities.
READ MORELearn about our programmes

Gaza
current
A ceasefire came into effect in Gaza on 19th January 2025. A surge of supplies has entered Gaza since the beginning of the ceasefire, enabling an increase in the humanitarian response to critical needs. Debris management, retrieval of bodies and addressing explosive ordnance contamination across Gaza are some of the immediate priorities, together with the further scaling up of humanitarian aid and reinstatement of essential services.
PLEASE HELP US RESPOND TO THE EMERGENCY IN GAZA
We have been supporting trauma care services in Gaza since 2009, most intensively since the 51 day war in 2014. Now another war, with hostilities beginning on 7th October 2023, is devastating Gaza and its people once again.
Our support for trauma services in Gaza has never been as needed as it is now.
Our experience in Gaza
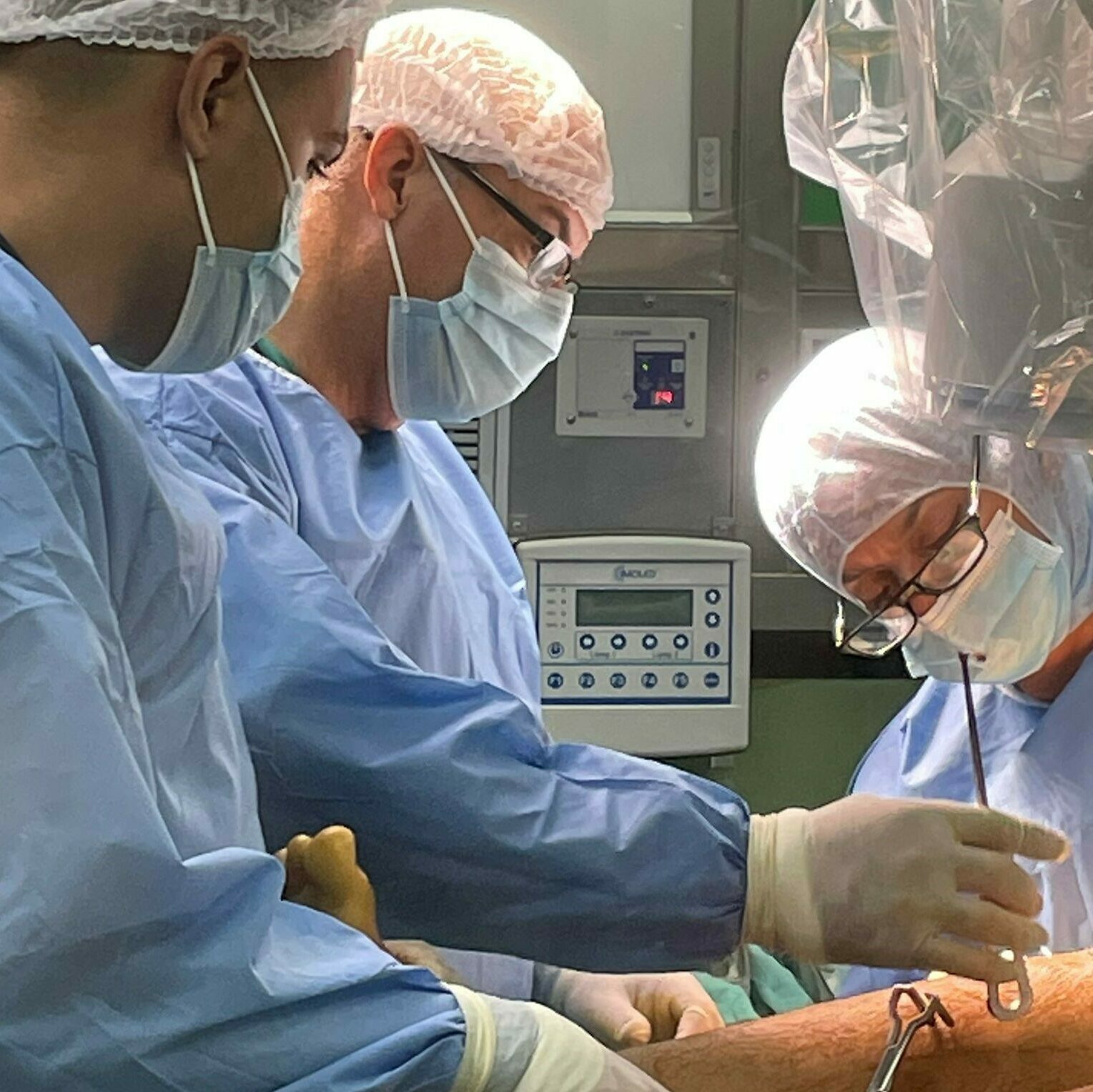
Dr Andy Ferguson spent two weeks working as a doctor in Gaza, at the European Hospital in Khan Younis, helping treat people with severe trauma wounds from bombing, shrapnel and gunfire.
As Israel's forces pushed further south into Gaza over Christmas and New Year, supplies of medicine, anaesthetic and crucial equipment began to run low - and eventually run out entirely in some places.
This is what Dr Ferguson saw.





